VTE/DVT/Filters
45 - Outcomes of Catheter-Directed Thromboembolectomy in ECMO-Treated Patients with Pulmonary Embolism: A Retrospective Study
Mohammad Jalili, MD – Resident physician, Radiology, Yale Bridgeport Hospital; Joshua Cornman-Homonoff, MD – Assistant Professor, Interventional Radiology, Yale School of Medicine
Purpose: This study evaluates the outcomes of catheter-directed mechanical pulmonary artery thromboembolectomy in critically ill patients receiving extracorporeal membrane oxygenation (ECMO).
Material and Methods: A retrospective analysis of patients treated for pulmonary artery embolism (PE) with ECMO within a multi-center healthcare system was performed. The patients were divided into two groups: those receiving catheter-directed pulmonary artery thromboembolectomy using the INARI FlowTriever system (FT) and those treated with anticoagulation (AC) alone. Baseline characteristics such as high-sensitive troponin, BNP, lactate, and hemoglobin were compared between the groups. Outcomes assessed included ICU length of stay (LOS), hospital LOS, and 30-day mortality.
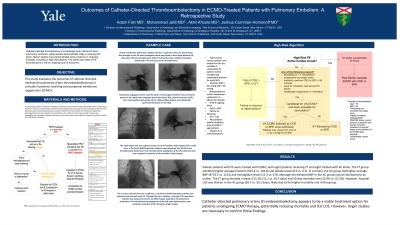
Results: Sixteen patients with PE were treated with ECMO, with eight patients receiving FT and eight treated with AC alone. The FT group exhibited higher average troponin (625.4 vs. 103.8) and lactate levels (8.3 vs. 6.3). In contrast, the AC group had higher average BNP (8753.3 vs. 1214) and hemoglobin levels (11.3 vs. 9.9), although the elevated BNP in the AC group may be attributed to an outlier. The FT group showed a lower ICU LOS (12.2 vs. 19.3 days) and 30-day mortality rate (25.0% vs. 62.5%). However, hospital LOS was shorter in the AC group (26.7 vs. 33.2 days), likely due to the higher mortality rate in this group.
Conclusions: Catheter-directed pulmonary artery thromboembolectomy appears to be a viable treatment option for patients undergoing ECMO therapy, potentially reducing mortality and ICU LOS. However, larger studies are necessary to confirm these findings.
Material and Methods: A retrospective analysis of patients treated for pulmonary artery embolism (PE) with ECMO within a multi-center healthcare system was performed. The patients were divided into two groups: those receiving catheter-directed pulmonary artery thromboembolectomy using the INARI FlowTriever system (FT) and those treated with anticoagulation (AC) alone. Baseline characteristics such as high-sensitive troponin, BNP, lactate, and hemoglobin were compared between the groups. Outcomes assessed included ICU length of stay (LOS), hospital LOS, and 30-day mortality.
Results: Sixteen patients with PE were treated with ECMO, with eight patients receiving FT and eight treated with AC alone. The FT group exhibited higher average troponin (625.4 vs. 103.8) and lactate levels (8.3 vs. 6.3). In contrast, the AC group had higher average BNP (8753.3 vs. 1214) and hemoglobin levels (11.3 vs. 9.9), although the elevated BNP in the AC group may be attributed to an outlier. The FT group showed a lower ICU LOS (12.2 vs. 19.3 days) and 30-day mortality rate (25.0% vs. 62.5%). However, hospital LOS was shorter in the AC group (26.7 vs. 33.2 days), likely due to the higher mortality rate in this group.
Conclusions: Catheter-directed pulmonary artery thromboembolectomy appears to be a viable treatment option for patients undergoing ECMO therapy, potentially reducing mortality and ICU LOS. However, larger studies are necessary to confirm these findings.
