VTE/DVT/Filters
17 - Chronic Veno-Occlusive Disease: Sharp Recanalization Techniques and Promising Outcomes
Kyle Cooper, MD – Associate Professor, Loma Linda University; Mina Makary, MD – Associate Professor, Ohio State Wexner Medical Center
Purpose: 1) Understand the etiology, pathophysiology, and clinical presentation of chronic veno-occlusive disease. 2) Present a detailed, image-rich case review of various sharp recanalization techniques used in treating chronic veno-occlusive disease. 3) Discuss the clinical outcomes associated with sharp recanalization. 4) Review the safety profile of sharp recanalization, including potential risks and management strategies.
Material and Methods: This presentation synthesizes current literature to explore the role of sharp recanalization in patients with chronic veno-occlusive disease including its role in the treatment paradigm, technical pearls, and evidence-based clinical outcomes. Treatment principles and techniques will further be illustrated through case-based examples.
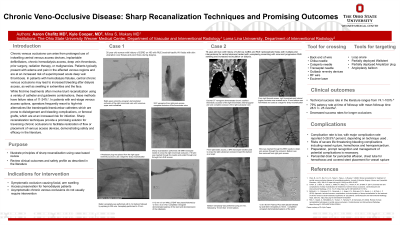
Results: Chronic venous occlusions can arise from use of indwelling central venous access devices, implantable defibrillators, chronic hemodialysis access, deep vein thrombosis, or malignancies. Patients typically present with edema and pain in the affected venous regions. In those undergoing hemodialysis, chronic venous occlusions may lead to increased bleeding after dialysis access, as well as swelling in extremities and the face.
First-line treatments with blunt recanalization can fail. Patients with end-stage venous access frequently resort to high-risk alternatives like transhepatic/translumbar catheters or femoral grafts, which pose infection risks. Sharp recanalization techniques provide a promising solution for traversing chronic occlusions, demonstrating safety and efficacy in the literature.
Techniques discussed include the use of the back end of stiff glidewires, needle-assisted recanalization methods (e.g., transseptal needles, TIPS access needles, Chiba needles), and devices such as the Outback re-entry device and radiofrequency wires. After successfully crossing the occlusion, venoplasty and stenting are performed. However, potential complications, including major bleeding events like pericardial effusion and hemothorax, require prompt identification and management.
Conclusions: This educational exhibit will enhance viewers' understanding of the indications, procedural techniques, clinical outcomes, and risks of sharp recanalization in patients with chronic veno-occlusive disease. Participants will gain insights into effective risk management strategies during these complex procedures, supported by image-rich case based examples.
Material and Methods: This presentation synthesizes current literature to explore the role of sharp recanalization in patients with chronic veno-occlusive disease including its role in the treatment paradigm, technical pearls, and evidence-based clinical outcomes. Treatment principles and techniques will further be illustrated through case-based examples.
Results: Chronic venous occlusions can arise from use of indwelling central venous access devices, implantable defibrillators, chronic hemodialysis access, deep vein thrombosis, or malignancies. Patients typically present with edema and pain in the affected venous regions. In those undergoing hemodialysis, chronic venous occlusions may lead to increased bleeding after dialysis access, as well as swelling in extremities and the face.
First-line treatments with blunt recanalization can fail. Patients with end-stage venous access frequently resort to high-risk alternatives like transhepatic/translumbar catheters or femoral grafts, which pose infection risks. Sharp recanalization techniques provide a promising solution for traversing chronic occlusions, demonstrating safety and efficacy in the literature.
Techniques discussed include the use of the back end of stiff glidewires, needle-assisted recanalization methods (e.g., transseptal needles, TIPS access needles, Chiba needles), and devices such as the Outback re-entry device and radiofrequency wires. After successfully crossing the occlusion, venoplasty and stenting are performed. However, potential complications, including major bleeding events like pericardial effusion and hemothorax, require prompt identification and management.
Conclusions: This educational exhibit will enhance viewers' understanding of the indications, procedural techniques, clinical outcomes, and risks of sharp recanalization in patients with chronic veno-occlusive disease. Participants will gain insights into effective risk management strategies during these complex procedures, supported by image-rich case based examples.
