VTE/DVT/Filters
48 - Clinical Deterioration And Therapy Escalation Events Following Pulmonary Embolism Intervention In The PEERLESS Trial
Purpose: PEERLESS (NCT05111613) is the first randomized trial to compare two interventions for pulmonary embolism (PE) and assess the incidence of in-hospital clinical deterioration and therapy escalation with different strategies.
Material and Methods: The trial enrolled 550 intermediate-risk PE patients randomized 1:1 to large-bore mechanical thrombectomy (LBMT; n=274) or catheter-directed thrombolysis (CDT; n=276). The primary endpoint was a hierarchal win ratio of all-cause mortality, intracranial hemorrhage, major bleeding, clinical deterioration and/or escalation to bailout therapy, and ICU utilization through discharge (max 7 days). Clinical deterioration events were adjudicated by an independent clinical events committee (CEC) and consisted of hemodynamic or respiratory worsening meeting prespecified definitions for severity and duration. Pragmatic therapy escalations were permitted contingent on review of patients’ holistic clinical status. Justifications for bailout were adjudicated by the CEC.
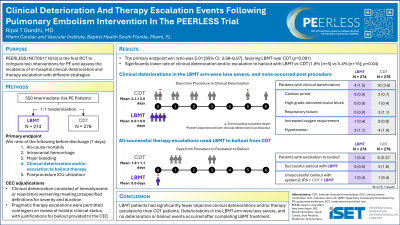
Results: The primary endpoint win ratio was 5.01 [95% CI: 3.68–6.97], favoring LBMT over CDT (p < 0.001). Assessment of win ratio components showed CDT patients had a significantly higher rate (5.4% [n=15] vs 1.8% [n=5]) of clinical deterioration and/or escalation to bailout vs LBMT patients (OR 3.09 [95% CI: 1.11–8.63]; p=0.04). Ten CDT (3.6%) and 4 LBMT (1.5%) patients experienced deteriorations. In the CDT arm, all deteriorations occurred after the procedure (2.3±2.0 overnights) including 2 cardiac arrests, 1 high-grade atrioventricular block, 3 respiratory failures, and 4 hypotension events. In the LBMT arm, all deteriorations were transient intraprocedural events (3 hypotension and 1 increased oxygen requirement). Seven patients at 6 study sites underwent bailout (6 CDT [2.2%] and 1 LBMT [0.4%]). In each arm, 1 patient underwent multiple unsuccessful bailout attempts. The remaining 5 CDT patients underwent successful bailout with LBMT 1.8±1.1 overnights post procedure due to a lack of clinical improvement and imaging confirmation of persistent PE after completing tPA infusion (16.6±3.1mg).
Conclusions: In PEERLESS, LBMT patients had significantly fewer objective clinical deteriorations and/or therapy escalations than CDT patients. Deteriorations in the LBMT arm were less severe, and no deterioration or bailout events occurred after completing LBMT treatment.
Material and Methods: The trial enrolled 550 intermediate-risk PE patients randomized 1:1 to large-bore mechanical thrombectomy (LBMT; n=274) or catheter-directed thrombolysis (CDT; n=276). The primary endpoint was a hierarchal win ratio of all-cause mortality, intracranial hemorrhage, major bleeding, clinical deterioration and/or escalation to bailout therapy, and ICU utilization through discharge (max 7 days). Clinical deterioration events were adjudicated by an independent clinical events committee (CEC) and consisted of hemodynamic or respiratory worsening meeting prespecified definitions for severity and duration. Pragmatic therapy escalations were permitted contingent on review of patients’ holistic clinical status. Justifications for bailout were adjudicated by the CEC.
Results: The primary endpoint win ratio was 5.01 [95% CI: 3.68–6.97], favoring LBMT over CDT (p < 0.001). Assessment of win ratio components showed CDT patients had a significantly higher rate (5.4% [n=15] vs 1.8% [n=5]) of clinical deterioration and/or escalation to bailout vs LBMT patients (OR 3.09 [95% CI: 1.11–8.63]; p=0.04). Ten CDT (3.6%) and 4 LBMT (1.5%) patients experienced deteriorations. In the CDT arm, all deteriorations occurred after the procedure (2.3±2.0 overnights) including 2 cardiac arrests, 1 high-grade atrioventricular block, 3 respiratory failures, and 4 hypotension events. In the LBMT arm, all deteriorations were transient intraprocedural events (3 hypotension and 1 increased oxygen requirement). Seven patients at 6 study sites underwent bailout (6 CDT [2.2%] and 1 LBMT [0.4%]). In each arm, 1 patient underwent multiple unsuccessful bailout attempts. The remaining 5 CDT patients underwent successful bailout with LBMT 1.8±1.1 overnights post procedure due to a lack of clinical improvement and imaging confirmation of persistent PE after completing tPA infusion (16.6±3.1mg).
Conclusions: In PEERLESS, LBMT patients had significantly fewer objective clinical deteriorations and/or therapy escalations than CDT patients. Deteriorations in the LBMT arm were less severe, and no deterioration or bailout events occurred after completing LBMT treatment.
